Seize the Moment, Collaborate on Research—Suggestions for Advancing COVID-19 Studies
Introduction:
Colleagues following the research progress of COVID-19 must be aware that in the clinical studies of COVID-19, a series of papers on clinical manifestations have been completed through the collaboration of clinical physicians from numerous hospitals. This is because everyone knows that a small number of cases cannot reflect the essence and patterns of the disease; the larger the sample size, the more it can reveal the true nature of the disease.
Similarly, in pathological research, the pathological manifestations and lesion patterns of many diseasesalso require observation, study, and summarization of a large number of cases to draw reliable conclusions.COVID-19 is now widely prevalent and is no longer a rare disease. Relying solely on the observation of individual cases can only provide a limited view, like looking at a leopard through a tube.Large-scale pathological studies of cases are imperative.
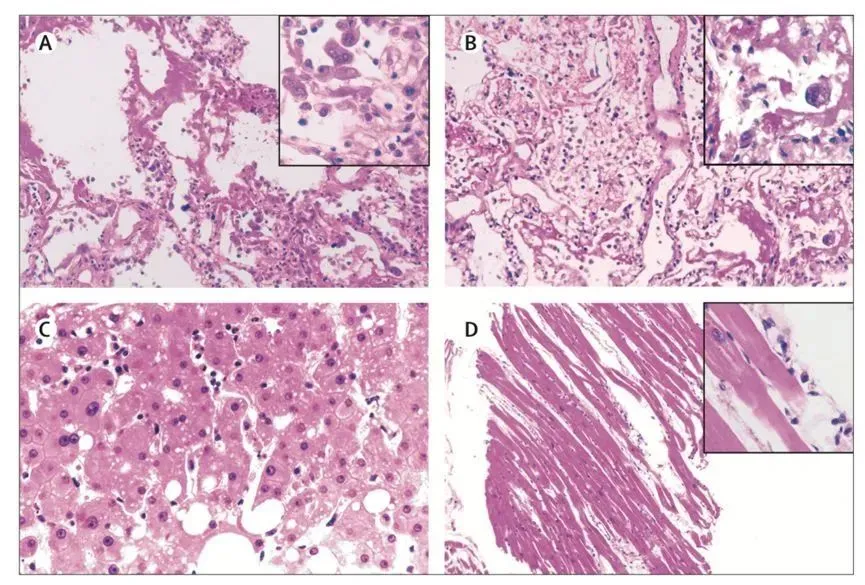
▲ Image of lung pathological manifestations in severe COVID-19 cases published in The Lancet
