In the previous installments of the immunohistochemical diagnosis series for renal epithelial tumors, we systematically introduced the immunohistochemical diagnostic aspects of multiple subtypes with clear cell morphology and eosinophilic/oncocytic cell morphology in renal tumors. In this issue,Wewillbased on a compilation of literature, we continue to introduce the application of immunohistochemistry in renal tumors with papillary formation morphology.

tumors with papillary formation
Papillary RCC (formerly type 1) and papillary adenoma
True papillary formation is common in renal tumors (Table 1), and papillary adenomas can be found in a considerable number of autopsy cases (76 out of 402 cases, 19%) (sometimes multifocal).
Table 1. Renal tumors with papillary architecture
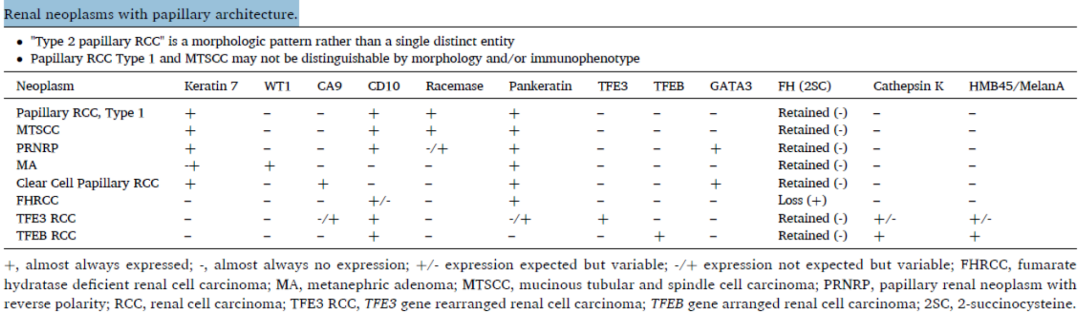
(Click to view larger image)
In both adult and pediatric patients, papillary RCC (previously described as type 1) is the second most common renal cell carcinoma, sharing the same histomorphological features with papillary adenoma, exhibiting papillary, tubular growth, occasionally solid growth, with bland tumor cells and typically monomorphic nuclei (Fig. 1A). Both are characterized by positive staining for AMACR (consistently strong/diffuse) (Fig. 1B), CK7 (Fig. 1C), CD10, and vimentin. The distinction between papillary adenoma and papillary renal cell carcinoma is primarily based on size (>15 mm). Necrosis in papillary RCC may be associated with CA IX positivity, but usually only focal near the necrosis. In large tissue sections, this differs from diffuse CCRCC.
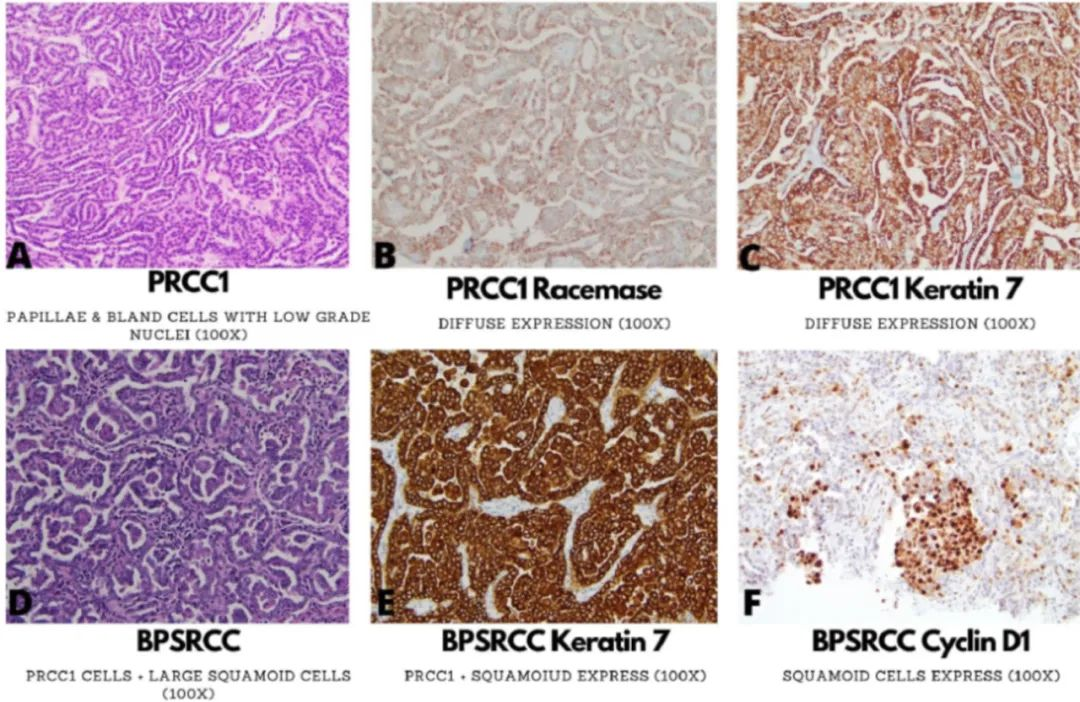
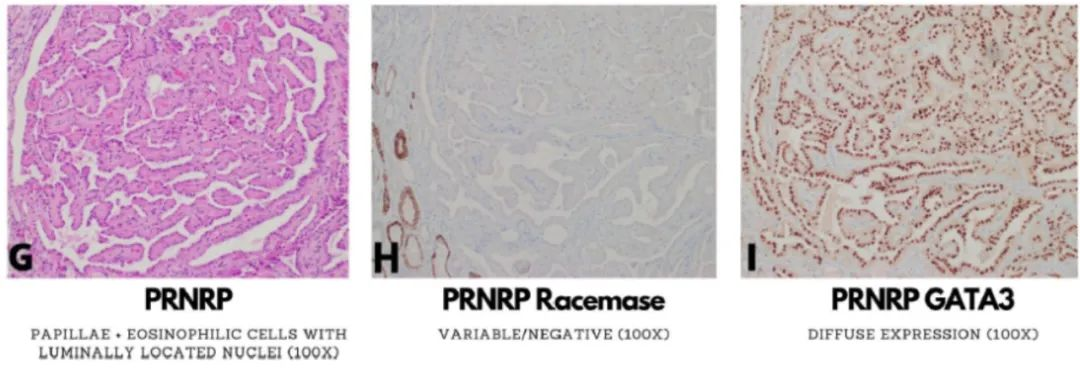
Fig. 1. Morphological and immunophenotypic features of type 1 papillary renal cell carcinoma (A-C), biphasic papillary and squamous renal cell carcinoma (BPSRCC; D-F), papillary renal neoplasm with reverse polarity (PRNRP; G-I).
New evidence suggests that the so-called biphasic papillary renal cell carcinoma (Fig. 1D) is a variant of type 1 renal cell carcinoma. This pattern consists of typical type 1 papillary tumor morphology with abundant eosinophilic epithelioid cells and frequent hobnail features. In the conventional morphological areas of this variant, CK7 (Fig. 1E) and AMACR are positive, while the larger epithelioid cells are positive for cyclin D1 (Fig. 1F).
Reference: Akgul M, Williamson SR. Immunohistochemistry for the diagnosis of renal epithelial neoplasms. Semin Diagn Pathol, 2022 Jan;39(1):1-16.




