Cyclooxygenase-2 (COX-2) is a rate-limiting enzyme in prostaglandin synthesis. Its gene, located on human chromosome 1q25.2-q25.3, is called PTGS2. It plays a key role in synthesizing important biological hormones: prostaglandins (PGs), such as PGE2, PGF2α, and thromboxane.
COX-2 is almost not expressed in normal tissues but is significantly expressed in most types of cancer tissues, including lung cancer, gastrointestinal cancer, breast cancer, head and neck cancer, hepatocellular carcinoma, etc. Overexpression of COX-2 can promote further carcinogenesis of cells, increase cancer recurrence rates, reduce patient survival rates, and mediate tumor cell resistance to treatment by producing excessive PGs.
Diagnostic and Prognostic Value of COX-2 Expression in Colorectal Cancer
Colorectal cancer is one of the leading causes of cancer-related deaths. The 5-year survival rate for patients with this disease generally does not exceed 20%. Therefore, effective and specific biomarkers are needed to determine the stage and type of colorectal cancer and evaluate patient prognosis.
Research by Benelli R et al. found that the percentage of tumors overexpressing COX-2 in colorectal adenocarcinoma, non-serrated adenoma, serrated polyps, and hyperplastic polyps was 85%, 60%, 25%, and 13%, respectively. In precancerous lesions, colorectal epithelial cells usually do not express COX-2 protein, but as the disease progresses, they gradually become positive (as shown in Figure 1). This indicates that COX-2 expression may be involved in the occurrence and development of colorectal cancer.
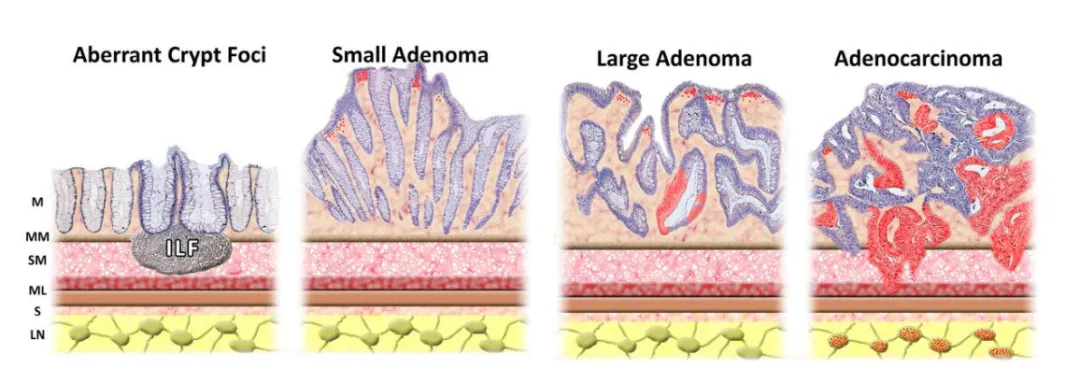
Figure 1. Expression of COX-2 in the Progression of Colorectal Cancer
M, Mucosa; MM, Muscularis Mucosa; SM, Submucosa; ML, Muscular Layer; S, Serosa; LN, Lymph Node. COX-2 positive areas/cells are highlighted in red.
Studies by Echizen K and Sun Peng et al. indicate that COX-2 mainly participates in the occurrence and development of colorectal cancer through the microenvironment: In the early stages of tumor formation, activation of the COX-2/PGE2 pathway induces the production of an inflammatory microenvironment. Subsequently, the inflammatory response in the stroma induces TNF-α signaling in tumor cells and activates the NOX1/ROS signaling pathway downstream, further driving tumorigenesis toward an irreversible direction.
Furthermore, in colorectal cancer cells, overexpressed COX-2 can increase the production of vascular growth factors, stimulate endothelial cell migration through the collagen matrix, form capillary-like networks, and reduce apoptosis by inhibiting the cytochrome C pathway through decreased Bcl-2 gene expression. By stimulating the EMT process, it increases cancer cell invasiveness and metastasis. Therefore, COX-2 overexpression is associated with the occurrence, development, and metastasis of colorectal cancer.
The study by Ma Jiachi et al. included 115 colorectal cancer patients. Immunohistochemistry was used to detect COX-2 expression levels. It was found that COX-2 expression rate in colon cancer tissues was higher than in normal colon tissues (p<0.05). Expression was lower in well-differentiated cancer tissues compared to poorly differentiated ones. COX-2 showed high expression in cases with lymph node metastasis. The later the tumor stage, the higher the COX-2 positive expression rate. COX-2 expression was not related to patient age, gender, lesion size, or liver metastasis (all P>0.05). Follow-up data on patients’ 5-year postoperative survival showed: The cumulative survival rate for COX-2 negative patients was 63.6%, while for positive patients it was 37.8%. Thus, COX-2 expression in colorectal cancer tissues can serve as an indicator for TNM staging and prognosis assessment.
Keisuke Kosumi et al. from the Dana-Farber Cancer Institute and the Department of Oncologic Pathology, Harvard Medical School, used the COX proportional hazards regression model to study 1708 colorectal cancer patients from stages I-IV. Immunohistochemistry was used to assess COX-2 expression status. They found a statistically significant interaction between COX-2 expression and patient BRAF mutation status: BRAF mutant patients with high COX-2 expression had lower survival rates than COX-2 negative patients, and survival rates decreased with increasing COX-2 expression (multivariate HR=2.44, 95% CI: 1.39-4.28). However, this phenomenon was not observed in the BRAF wild-type control group (multivariate HR=0.82, 95% CI: 0.65-1.04). This indicates that in colorectal cancer patients with BRAF mutations, tumor COX-2 expression status is an effective biomarker for prognosis prediction.
COX-2 Expression as a Biomarker for Immunotherapy
In the tumor microenvironment (TME), COX-2-derived PGE2 can help transform the TME from an anti-tumor response to an immunosuppressive response in various ways, becoming an accomplice in cancer cell immune escape. Therefore, the combination of COX-2 inhibitors and ICIs is a potential immunotherapy option, as validated in experiments by Zelenay S et al. Compared to anti-PD-1 antibody alone, the combination of COX-2 inhibitors (including NSAIDs and specific COX-2 inhibitors) with anti-PD-1 antibodies better promoted tumor regression. In this process, COX-2 expression level is an effective marker for predicting and prognosticating immunotherapy efficacy.
Related Antibodies from Maixin
|
Antibody Name
|
Product Number
|
Clone Number
|
Positive Location
|
|
COX-2
|
RMA-0549
|
SP21
|
Cytoplasm/Cell Membrane
|
References:
[1]Benelli R, R Venè, Ferrari N. Prostaglandin-endoperoxide synthase 2 (cyclooxygenase-2), a complex target for colorectal cancer prevention and therapy[J]. Translational Research the Journal of Laboratory & Clinical Medicine, 2018:S1931524418300033.
[2]Echizen K , Oshima H , Nakayama M , et al. The inflammatory microenvironment that promotes gastroin-testinal cancer development and invasion.[J]. Advances in Biological Regulation, 2018:S2212492618300721
[3] Sun Peng, Quan Jichuan, Guan Xu, et al. The Relationship Between Cyclooxygenase-2 and Colorectal Cancer and Progress in Its Targeted Therapy [J]. Journal of Oncology, 2019(12):1031-1036.
[4] Ma Jiachi, Zhao Xiaodan, Qi Jianbo, et al. Expression and Clinical Significance of Prostaglandin E2 and Cyclooxygenase-2 in Colorectal Cancer Tissues [J]. Chinese Journal of General Surgery, 2018, 33(04): 322-325.
[5]Kosumi K, Hamada T, Zhang S, et al.Prognostic association of PTGS2 (COX-2) over-expression according to BRAF mutation status in colorectal cancer: Results from two prospective cohorts and CALGB 89803 (Alliance) trial. Eur J Cancer. 2019 Apr:111:82-93.
[6]Pu D, Yin L, Huang L, et al. Cyclooxygenase-2 Inhibitor: A Potential Combination Strategy With Immunotherapy in Cancer[J]. Frontiers in Oncology, 2021, 11:637504.


