A Conversation on Etiological Diagnosis
Preface:
Not long ago, due to the etiological diagnosis of a rare case, I intermittently discussed with several netizens skilled in microbiological examination on WeChat for a whole morning. This was a case of coccidioidomycosis, primarily caused by Coccidioides immitis infection. This disease is more common in the Americas, especially the southwestern United States; there are also a few sporadic cases in China. As of the end of 2018, only over 30 cases had been reported domestically, some of whom had traveled to areas where coccidioidomycosis is endemic.
This disease is mainly transmitted via the respiratory route, often occurring in populations with lower immune defense capabilities. It primarily affects the respiratory tract but can also disseminate, involving tissues such as the skin, central nervous system, kidneys, bones, and lymph nodes. The main lesions are suppurative and granulomatous. Etiological diagnosis can employ methods such as direct microscopic examination of specimens, histopathological examination, fungal culture, serological testing, and coccidioidin skin test. In terms of pathology, diagnosis is based on finding typical Coccidioides in the lesional tissue. Because it is quite rare, not only are many people in the microbiology department of the laboratory unfamiliar with it, but few pathologists know about it either. However, due to its distinctive morphology, once seen, it can be recognized. The author happened to encounter a case and, feeling it was special, consulted many Chinese and foreign literature, compared dozens of Chinese and foreign images, and finally confirmed Coccidioides. Therefore, I had some confidence and discussed it with several microbiology experts.
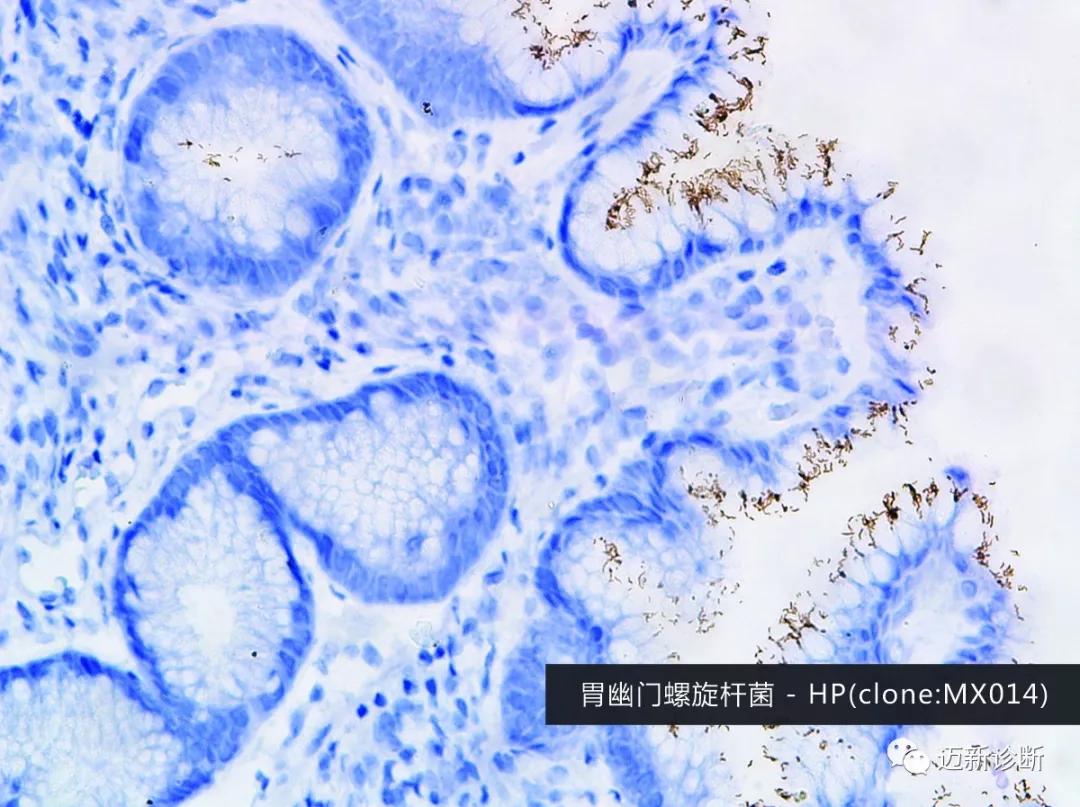
Immunohistochemistry, H. pylori positive
